Click here to comment on YouTube
T-cells play a crucial role in the adaptive immune response – our ability to recognize specific antigens on foreign invaders like pathogens. In this post, we’re going to look at how they develop.
T-Cell Development in Bone Marrow
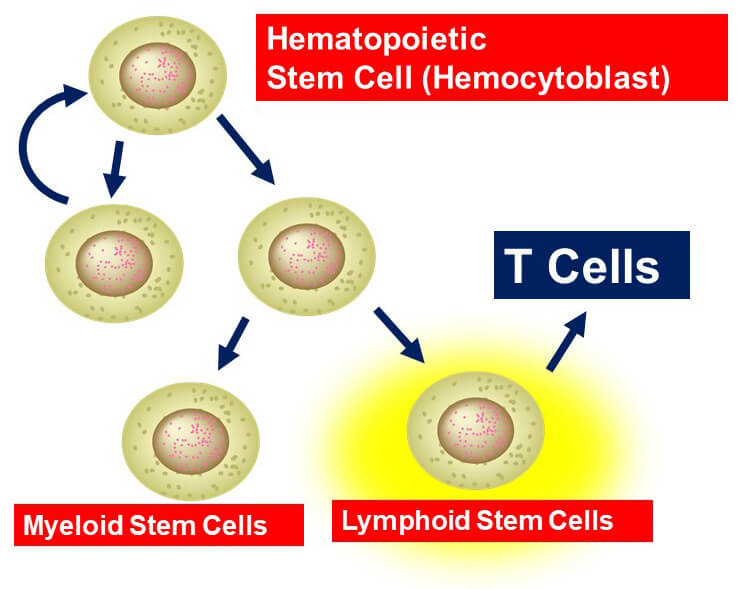
T-cells start their developmental journey in the Bone Marrow. We begin with hematopoietic stem cells that go through a lot of division and differentiation to become all of the cell types in the blood.
In that process, they can either differentiate into a myeloid stem cell or a lymphoid stem cell. And it’s from the lymphoid stem cell that we ultimately get the T-cells. Check out our post on hemopoiesis for a detailed review of that process.
T-Cell Maturation in the Thymus
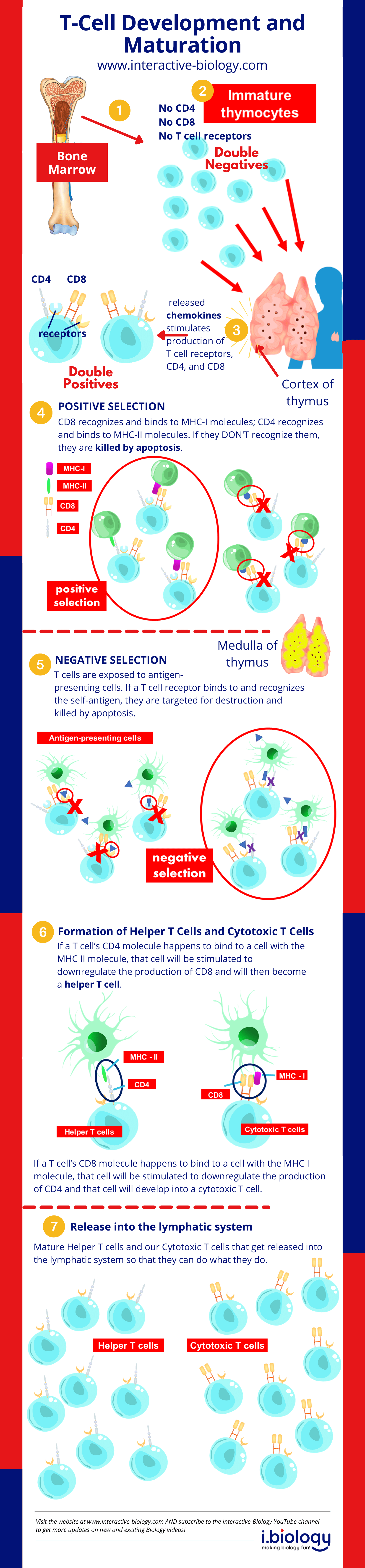
While T-cells start their development and differentiation in the bone marrow, they don’t finish the process there. When they leave the bone marrow, immature thymocytes need to go to the thymus to mature into fully functioning T-cells. It’s like they are training to be military fighters, but before they can go off to fight, they first need to go to Bootcamp to go through some training and to weed out those that don’t cut it. The “Bootcamp” happens in the thymus, and every T cell won’t make it. Let’s look at how this happens.
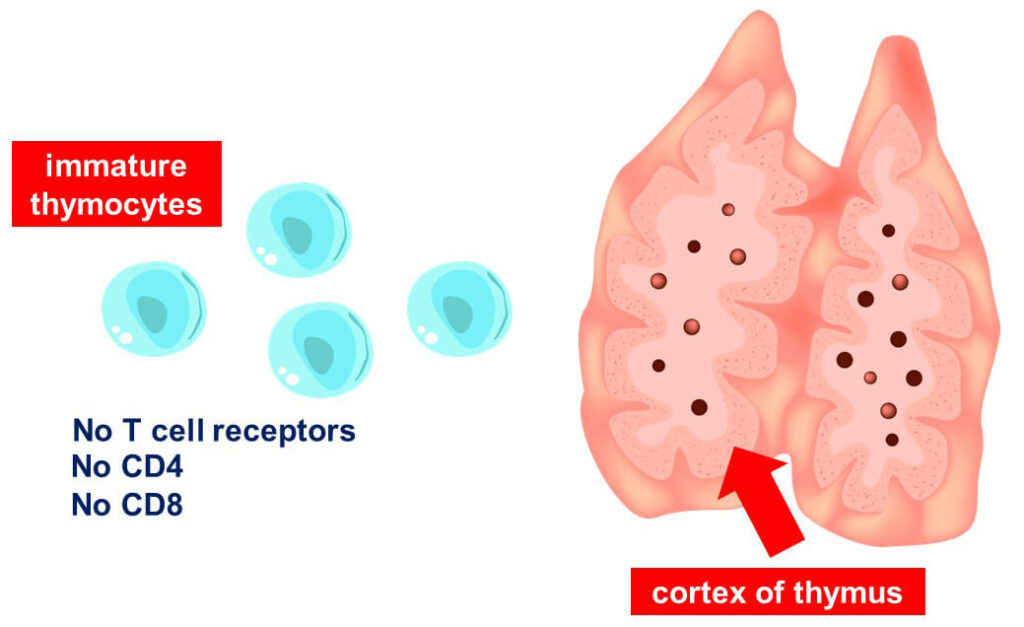
The thymus secretes certain chemicals that act as chemokines. Those chemicals attract the immature T-cells to it to go through the maturation process.
The maturation process starts in the cortex of the thymus. These immature T-cells don’t have T cell receptors (TCRs) on their surfaces, nor do they have two vital molecules – CD4 and CD8. We classify these as double negatives.
CD4 and CD8 Production and Positive Selection
The thymus releases chemicals that stimulate the T-cells to produce T-cell receptors (or TCRs). They will also stimulate the T-cells to produce CD4 and CD8. All of this happens by activating the genes responsible for producing these proteins. At this stage, the T-cells now have TCRs and both CD4 and CD8. The cells are now considered double positive.
We now need to see if the CD4 and CD8 will bind to two molecules on the thymic epithelial cells. CD8 is supposed to recognize and bind to MHC-I molecules, and CD4 is supposed to recognize and bind to MHC-II molecules. If they don’t recognize them for some reason, they are killed by apoptosis. They are no good, so we get rid of them.

If they bind to the MHC molecules, they can move on to the next step. This is called positive selection. If it binds, we want them, so we keep them.
Negative Selection
From here, the T cell will then go a little deeper and move to the medulla of the thymus – where the next step takes place. The T-cells are then exposed to self-antigens. Now, we don’t want t-cells to recognize and bind to antigens that are supposed to be present in the body, so here’s how we accomplish this.

Self-antigens from other parts of the body are brought to the thymus by antigen-presenting cells. If a T cell receptor binds to and recognizes the self-antigen, they are targeted for destruction and killed by apoptosis. This is called negative selection. We are killing off T-cells that recognize antigens of our own body tissues because we don’t want T-cells to start attacking our tissues – well, at least not under normal circumstances.
So, we had positive selection for T-cells with CD4 and CD8 molecules that successfully recognized MHC I and II and negative selection to only get T-cells that WON’T recognize our normal body cells.
Helper T-Cells and Cytotoxic T-Cells
The next thing that happens is the T-cells are then exposed to other body cells. Some of those cells will have MHC I molecules on their surface, and some will have MHC II molecules. If a T cell’s CD4 molecule happens to bind to a cell with the MHC II molecule, the T cell will be stimulated to downregulate the production of CD8. This cell will then become a helper T cell. The presence of CD4 characterizes helper T-cells.

Now, if a T cell’s CD8 molecule happens to bind to a cell with the MHC I molecule, that cell will be stimulated to downregulate the production of CD4, and that cell will develop into a cytotoxic T cell. This is a random process. Whatever it binds to will determine what is expressed, what is reduced, and what it becomes.
And now, we have our mature Helper T-cells and our Cytotoxic T-cells that get released into the lymphatic system so that they can do what they do.
Infographic