In continuation of my article from last week I want to dig a little deeper into the mechanism of the regulation of blood pressure. Last week, we stated that the two divisions of the Autonomic Nervous System (Sympathetic and Parasympathetic Nervous systems) were the conduits through which blood pressure is controlled, which is the most rapidly responding regulator of blood pressure.
The Autonomic Nervous system receives continuous information from the baroreceptors (pressure sensitive nerve endings) situated in the carotid sinus and aortic arch. These are extrinsic factors along with hormones that control blood pressure. While there are also local intrinsic controls such as metabolic controls that facilitate certain needs the body demands by controlling how quickly or slowly the item is transported by influencing the pace of blood pressure.
The Determinants and Their Control
Mean arterial pressure depends on Cardiac Output (CO) and Total Peripheral Resistance (TPR). Just to recap, cardiac output is the volume of blood being pumped by the heart, in particular by a left or right ventricle in the time interval of one minute. While peripheral resistance is the sum of all the blood vessels in systemic circulation.
A number of factors, in turn, determine cardiac output and peripheral resistance. After we go through these factors you will be able to fully appreciate the complexity of blood pressure regulation, reviewing all factors that go into determining mean arterial pressure. We will pull them all together.
[unordered_list style=”arrow”]
- Mean arterial pressure is dependent on cardiac output and peripheral resistance.
- CO depends on heart rate and stroke volume.
- Heart Rate depends on the relative balance of the parasympathetic activity, which decreases heart rate (acts as the brake pedal in this pathway as mentioned in the previous article), and sympathetic activity which increases heart rate (which acts as the gas pedal in this pathway).
- Stroke volume increases to sympathetic activity.
- Stroke volume also increases as venous return (deoxygenated blood) increases to heart.
- Venous return is enhanced by sympathetically induced venous vasoconstriction, skeletal muscle pump, respiratory pump and cardiac suction.
- The effective circulating blood volume also influences how much blood is returned to the heart. The blood volume depends in the short term on the size of passive bulk0flow fluid shifts between plasma and interstitial fluid across capillary walls. In the long term, the blood volume depends on salt and water balance which are hormonally controlled by the RAAS (Renin-Angiotensin-Aldosterone System) and vasopressin, respectively
- TPR, the other major determinant of mean arterial pressure, depends on the radius of all arterioles as well as blood viscosity. The main factor determining blood viscosity is the number of red blood cells, however arteriolar radius is more important than viscosity.
- Arteriolar radius is influenced by intrinsic factors, that means locally. There are metabolic controls that match blood flow with metabolic needs. For example, local changes that take place in active skeletal muscles cause local arteriolar vasodilation and blood flow is increased to these muscles.
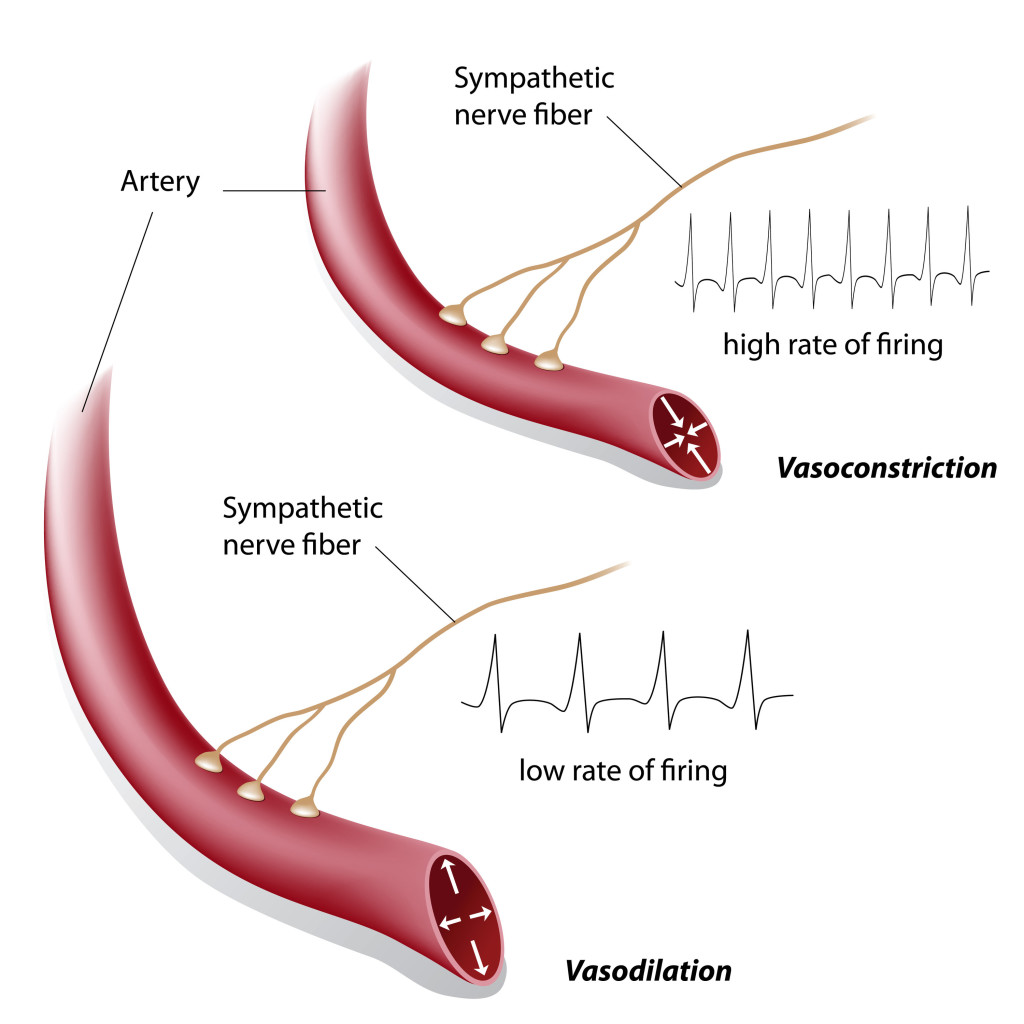
- Arteriolar radius is also influenced extrinsically by sympathetic activity, a control mechanism that causes arteriolar vasoconstriction to increase TPR and mean arterial blood pressure.
- Arteriolar radius is also extrinsically controlled by hormones that control vasoconstriction such as vasopressin and angiotensin II as well as being important to salt and water balance.
Changing any one of these important factors will change the blood pressure, unless there is a compensatory change in another variable that would keep the blood pressure constant.
The final installment to this series will complete the understanding of blood pressure regulation speaking towards short-term and long-term control measures and the baroreceptor reflex mechanism specifically.

thanks alot this page is splendid
can you please explain haemodynamics ?? pleaseeeeeee
Thank you for your comments I can try but it wouldn’t be uploaded for another 2 weeks and I don’t know how quickly I’ll be able to do so. But I will try and write about it after I complete this series with the 3rd and final installment on blood pressure.