What is Erythropoiesis?
Because of the inability of erythrocytes (red blood cells) to divide to replenish their numbers, the old ruptured cells must be replaced by totally new cells. They meet their demise because they don’t have the usual specialized intracellular machinery, which controls cell growth and repair, leading to a short life span of 120 days.
This short life span necessitates the process erythropoiesis, which is the formation of red blood cells. All blood cells are formed in the bone marrow. This is the erythrocyte factory, which is soft, highly cellular tissue that fills the internal cavities of bones.
During intrauterine development, the early stages of life, erythrocytes are produced first by the yolk sac and then by the developing spleen during the third month of gestation, until the bone marrow is formed in the seventh month and takes over erythrocyte production exclusively.
Erythrocyte Differentiation
Erythrocyte differentiation takes place in 8 stages. It is the pathway through which an erythrocyte matures from a hemocytoblast into a full-blown erythrocyte. The first seven all take place within the bone marrow. After stage 7 the cell is then released into the bloodstream as a reticulocyte, where it then matures 1-2 days later into an erythrocyte. The stages are as follows:
- Hemocytoblast, which is a pluripotent hematopoietic stem cell
- Common myeloid progenitor, a multipotent stem cell
- Unipotent stem cell
- Pronormoblast
- Basophilic normoblast also called an erythroblast.
- Polychromatophilic normoblast
- Orthochromatic normoblast
- Reticulocyte
There are four major steps in erythropoiesis, which I will explain.
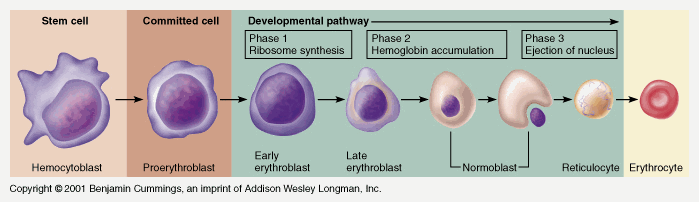
Erythrocytes are derived in the red bone marrow from pluripotent stem cells that give rise to all types of blood cells. Myeloid stem cells are partially differentiated cells that give rise to erythrocytes and several other types of blood cells.
Nucleated erythroblasts are committed to becoming mature erythrocytes. These cells extrude their nucleus and organelles, making more room for hemoglobin. Reticulocytes are immature red blood cells that contain organelle remnants. Mature erythrocytes are released into the capillaries. The pictures in this link and here show the steps of differentiation.
Distinct Characteristics of Erythrocytes during Erythropoiesis
These characteristics can be seen during erythrocyte maturation:
- The size of the cell decreases
- The cytoplasm volume increases
- Initially, there is a nucleus and as the cell matures the size of the nucleus decreases until it vanishes with the condensation of the chromatin material.
Regulation of Erythropoiesis
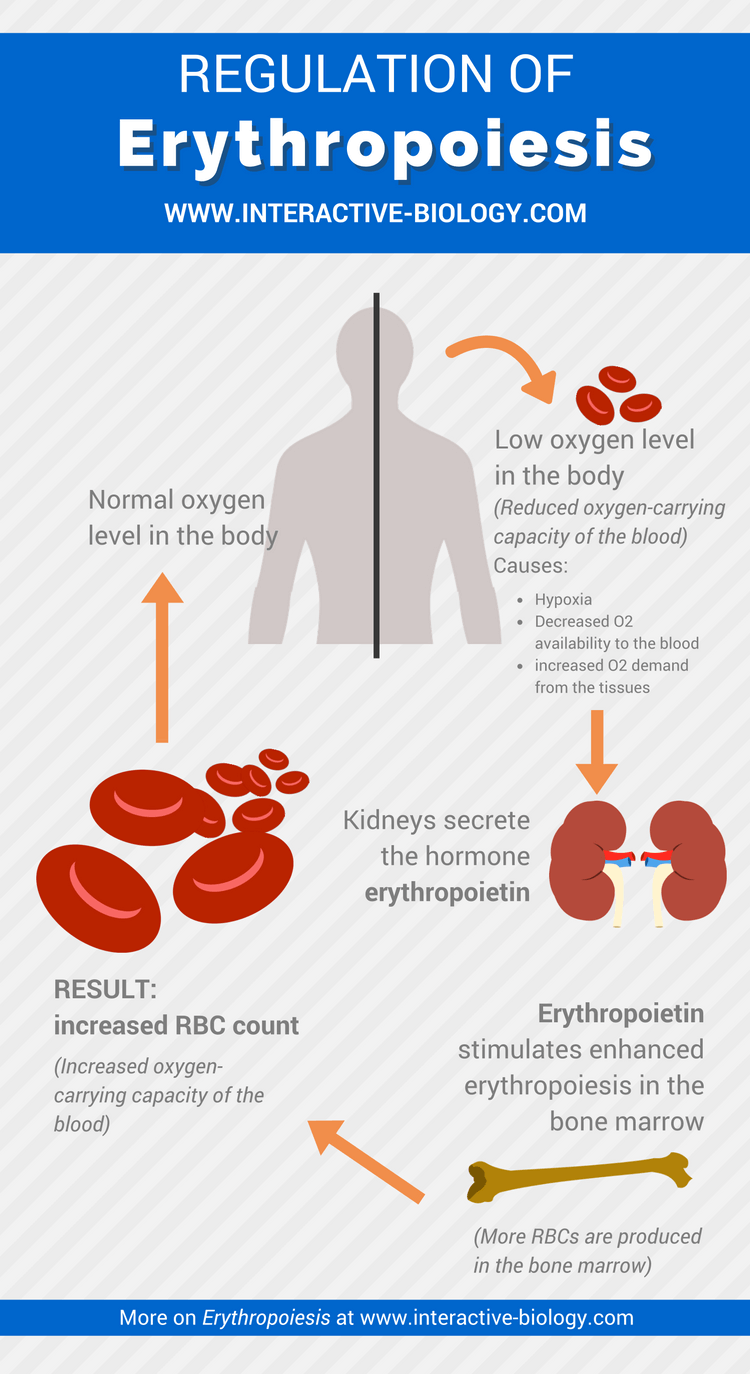
Thinking logically, you might suspect that because the primary function of erythrocytes is to transport oxygen in the blood, the primary stimulus for erythrocyte production is low oxygen levels. You would be correct, but low oxygen levels do not stimulate erythropoiesis by acting directly on the bone marrow.
Instead, it stimulates the kidneys to secrete the hormone erythropoietin into the blood, and this hormone in a domino effect stimulates the bone marrow to produce erythrocytes.
Erythropoietin acts on derivatives of undifferentiated cells that have already been committed to becoming red blood cells (RBC’s), stimulating the proliferation and maturation of these cells into mature RBCs.
This increase in erythropoietic activity elevates the number of circulating RBCs, thereby raising the oxygen-carrying capacity of the blood and restoring the delivery of oxygen to the body tissues to normal. Once the oxygen level in the tissues of the kidneys is brought back to normal, erythropoietin secretion is turned down until it is needed again. This is an example of a negative feedback mechanism.
Infographic


It was a comprehensive explanation, Thank you. It helped me clear my concept.
I love this site….. it helps alot. Thank you.
Could you clarify? In the fetus, are red blood corpuscles formed in the spleen or the liver?
Thanks very much and good luck in Medical School!
Pam
It is both the spleen and the liver the liver participates more in this exercise than the spleen, I am now noticing that the liver was left out, but the liver is the major contributor and is assisted by the spleen in the fetus. Sorry for that error hope this is cleared up for you and will try to get that corrected .
Paul
Can liver take part in formation of any blood cell in in human body. In the age of ten spleen take part in formation of RBCs.
Thanks dear,
This is a very vital info,however,I would love it more if you could add in some functions,
clear structures,destruction process and replications.
Thanks again.
all the best
am a ghanaian nursin student in ma final year……i wish to be in the medical school one time in ma life
Thanque soooo much help of these theory i have learned so much…
Regarding the derivation of erythrocytes from the bone marrow, I am confused because I thought that multipotent stem cells, such as the hematopoietic stem cell, were the progenitors of erythrocytes. Are there also pluripotent stem cells present in the bone marrow?
I appreciate how u explained this process very well and clear in the understandable way>
Thanks a lot again
Now i can explain the process very well.
u did it well.
A very helpful piece indeed! Thanks a lot! I’ve just used it to put my presentation together.
good one……………………….
i understood erythrocytes perfectly well
thanks for da help
i shubhankar want’s to know about erythropoiesis – megaloblastic maturation seen and the test has been occurred on 15th may 2014.i want to know the remedies and the solutions.
its aowsome im write a note on the genesis of blood an these has help me alot on the rbc aspect of my note thank alot.
Ensure it’sn’t going to interfere with every other
outside devices or structures you’ve. Another wonderful point about Shield
Ak is the fact that it is an environmentally safe squirt.
What a educating site!!!!!!!
I love this site
nice information, well erythropoiesis controlled by erythropoietin hormone by kidney
plz could u tell me where the rbc’s are produced in newborns and adults
@dr.mehnaaz yaqoob starting with the yolk sac, then the spleen and liver, then the skeleton
In early fetus, they r produced in the mesodermal cells of the yolk sac..moves to liver n spleen in 3month then to bone marrow by 7 month
Hemocytoblast is pluripotent nt multipotent
what of the spleen?
Excellent article .Good for mbbs students
@dr.mehnaaz yaqoob
in embryo rbcs are born in connective tissue
then after some time convert to liver
and then convert to bone marrow in adult